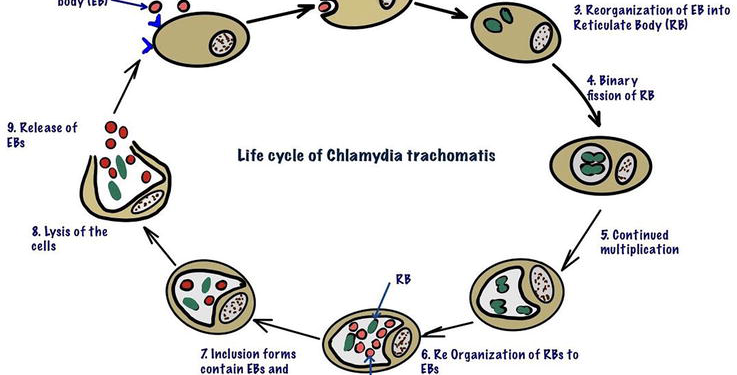
Chlamydia trachomatis infection is one of the most common sexually transmitted infections (STIs) worldwide, particularly affecting the urogenital tract. Despite its prevalence, it is often asymptomatic, allowing it to spread silently and cause long-term complications such as infertility, pelvic inflammatory disease, and chronic pelvic pain. With the development of molecular diagnostics, RNA-based testing using transcription-mediated amplification (TMA) has emerged as a highly sensitive and specific method for detecting Chlamydia trachomatis in urogenital specimens.
This article explores the concept of Chlamydia trachomatis RNA TMA urogenital testing, its methodology, clinical uses, advantages, and its role in modern sexual health diagnosis.
Understanding Chlamydia trachomatis
Chlamydia trachomatis is a gram-negative intracellular bacterium that primarily infects the epithelial cells of the urogenital tract. It is spread through sexual contact and can affect both men and women. Common sites of infection include:
Cervix (in women)
Urethra (in both sexes)
Rectum and throat (in some cases)
A major challenge in controlling this infection is that 70-80% of women and 50% of men may remain asymptomatic, making routine screening essential.
What is RNA TMA testing?
Transcription-mediated amplification (TMA) is a nucleic acid amplification test (NAAT) designed to detect RNA targets rather than DNA. Unlike traditional PCR methods, TMA amplifies ribosomal RNA (rRNA), which is present in high copy numbers in bacterial cells.
Key features of TMA:
Targets RNA instead of DNA.
Isothermal amplification (no thermal cycling required)
Sensitivity due to abundant RNA
Rapid and efficient detection
When applied to urogenital specimens, TMA can accurately identify active Chlamydia trachomatis infection.
Why is RNA focused on in urogenital testing?
RNA-based detection has several advantages:
1. Indication of active infection
RNA degrades rapidly after bacterial death, so RNA detection suggests viable organisms rather than residual genetic material.
2. Increased sensitivity
Because each bacterial cell contains thousands of RNA molecules, TMA can detect infection even with very low bacterial loads.
3. Improved clinical accuracy
RNA detection reduces false positives that can occur with DNA-based tests that detect non-viable bacteria.
Urogenital Specimen Types
For Chlamydia trachomatis RNA TMA urogenital testing, several specimen types are commonly used:
Urine specimens (especially first-pass urine)
Vaginal swabs (self-collected or clinician-collected)
Endocervical swabs
Urethral swabs
Self-collected vaginal swabs are particularly valuable because they are less invasive and have greater sensitivity than specimens collected by clinicians.
Clinical Applications
1. Routine Screening
TMA testing is widely used in screening programs, particularly:
Sexually active women under 25 years of age
Individuals with multiple partners
High-risk populations
2. Diagnosis of symptomatic patients
Patients who present with symptoms such as discharge, dysuria, or pelvic pain may benefit from accurate RNA-based detection.
3. Therapeutic test (selective use)
In some cases, such as pregnancy or persistent symptoms, TMA can help determine whether the infection has cleared.
4. Detection of co-infections
Many testing platforms allow for the simultaneous detection of other pathogens such as Neisseria gonorrhoeae, increasing diagnostic efficiency.
Advantages of TMA over other methods.
High sensitivity and specificity
Compared to older methods such as culture or antigen detection, TMA offers improved diagnostic performance.
Faster turnaround time
Results can often be obtained within hours, accelerating clinical decisions.
Non-invasive testing options
Urine and self-collected swabs reduce discomfort and improve patient compliance.
Scalability for public health programs
TMA is suitable for large-scale screening due to its automation capabilities
Limitations and Precautions
Although TMA is highly effective, there are some precautions:
Cost
Molecular testing can be more expensive than traditional methods, which may limit access in low-resource settings.
Technical Requirements
Requires specialized laboratory equipment and trained personnel.
RNA Stability.
Although RNA detection indicates active infection, improper handling of the sample can lead to degradation and false negatives.
Public Health Impacts.
The use of Chlamydia trachomatis RNA TMA urogenital testing has significantly improved STI control efforts by:
Increasing early detection
Reducing transmission rates
Preventing long-term complications
Supporting targeted treatment strategies
Screening programs that incorporate TMA testing have increased case detection rates, particularly among asymptomatic individuals.
Future Perspectives
The future of chlamydia diagnosis is moving towards:
Rapid, point-of-care RNA testing for same-visit results
Multiplex assays detect multiple pathogens simultaneously
Integration with digital health systems for tracking and reporting
Expanded self-testing options to increase accessibility
Advances in molecular biology continue to improve RNA amplification technologies, making them more affordable and widely available
Conclusions.
Chlamydia trachomatis RNA TMA urogenital testing represents a significant advance in the diagnosis and management of one of the world’s most common sexually transmitted infections. By targeting RNA, this method provides a more accurate indication of active infection, improves sensitivity, and supports effective treatment decisions.
As healthcare systems continue to prioritize early diagnosis and prevention, RNA-based TMA testing will play a critical role in reducing the global burden of chlamydia and improving reproductive health outcomes.